
For people living with diabetes, the condition can dramatically impact all aspects of their lives. People understand that diabetes can cause serious medical complications such as heart and kidney problems, but there is also a potential link between diabetes and brain injury.
Despite this evidence, there remains limited knowledge about the actual connection between diabetes and long-term brain health, so we decided to explore this issue in further detail.
In this blog post, we will discuss what research has revealed regarding the effects of chronic hyperglycemia on the central nervous system. How it could be a significant contributor to age-related cognitive decline, and elderly patients are particularly vulnerable due to stroke or head trauma occurring from slips/trips or falls.
Diabetes mellitus is a condition that hinders cellular mitochondria from efficiently using glucose, the body’s natural and brain’s primary source of energy. It is a chronic health condition characterized by the body’s inability to regulate blood sugar levels.
It occurs when the pancreas either fails to produce enough insulin or cannot use the insulin it produces effectively, resulting in increased levels of glucose in the bloodstream. This can lead to serious health complications, including heart disease, kidney failure, blindness, stroke, nerve damage, and lower limb amputations.
People with diabetes may also experience fatigue, frequent urination, excessive thirst and hunger, and blurred vision. In extreme cases, it can even be life-threatening if left untreated. Diabetes Mellitus is one of the most common chronic diseases worldwide and affects over 422 million people globally.
Diabetes mellitus may have any of 2 types:
There is a severe lack of insulin since the pancreas hardly makes any. The hormone insulin facilitates glucose use by cells. Without insulin, glucose would be unable to gain entry into the cells.
This kind of diabetes is characterized by insulin production by the pancreas. But alas, it either doesn’t produce enough, or the insulin is ineffective. Having this kind of is synonymous with insulin resistance. Almost all diabetics suffer from type 2, which accounts for 90% of cases.

Diabetes has a mysterious origin that has yet to be determined. Yet, there are things like:
Sugar, in and of itself, does not contribute to the development of diabetes, despite what many people believe. Diabetes is not one of those disorders that a sugary diet may bring on. Nonetheless, if a diabetes diagnosis has been made, it is suggested that sugar consumption be closely monitored.
The following are some of the symptoms of diabetes mellitus:
Traumatic Brain Injury (TBI), or intracranial injury, is an injury to the brain caused by an external force such as a blow or jolt to the head. It can also be caused by an object penetrating the skull and entering the brain tissue. It can occur at any age, although it is most common in younger individuals involved in contact sports or car accidents.
TBI can lead to a range of physical and psychological difficulties with varying levels of severity depending on the amount of damage inflicted upon the brain. Symptoms range from mild confusion, dizziness, blurred vision, coordination problems, and headaches to mood swings, seizures, and impaired cognitive functions such as memory loss. In extreme cases, coma or death may result.
Treatment for TBI depends on the source and degree of injury incurred. Milder forms may require rest with periodic checkups, while more severe cases may need surgery to remove objects from the skull or repair damage to brain tissue.
Physical therapy may help improve coordination and balance, while speech therapy is useful for language-related difficulties. Occupational therapy focuses on assisting patients in returning to their pre-injury lives by developing skills in a school or work-relevant activities such as problem-solving and self-care tasks.
Psychological support is also crucial for people suffering from TBI since it helps them cope with emotions associated with changes in their lifestyle due to their condition.
Neuroendocrine diseases may have an impact on glucose control, and they can result in brain damage, albeit this is relatively uncommon. As a result, certain individuals may be at risk for developing Type 2 diabetes.
Diabetic complications might be made worse by a brain injury. This is due to the fact that following an injury, the body produces stress hormones to aid in the battle against infection and other health issues. In addition, elevated blood sugar levels may result from the hormones’ effect of decreasing insulin sensitivity.
The condition of hyperglycemia might manifest itself if the levels get too high in a patient. If left untreated, hyperglycemia is associated with cognitive impairment and may have catastrophic consequences, including death.
However, untimely insulin administration might worsen diabetes’s effects on the brain. Diabetic comas may be brought on by either high or low blood sugar levels, resulting in permanent brain injury if not managed. Brain trauma is another possible outcome of a diabetic seizure brought on by very low blood sugar levels.
The primary focus of diabetes therapy is to maintain stable blood glucose levels. Altering your diet and taking insulin shots are both effective methods.
In order to prevent dangerous swings in blood sugar levels, people with diabetes must diligently check their levels frequently. In addition, since the pancreas of a person with type 1 diabetes does not create any insulin on its own, it will require insulin injections on a routine basis as well.
Most people with type 2 diabetes are able to keep their disease under control by eliminating sugary meals and increasing their physical activity. Extra glucose may be burned off during a workout, which aids in maintaining steady levels of glucose in the blood. Patients may sometimes need additional insulin injections.
Diabetes management can be particularly challenging if a person has a brain injury. Since your memory isn’t what it used to be, forgetting to check your glucose levels or give yourself insulin is a real possibility.
If you’ve suffered a brain injury, don’t worry about being reliant on others to take care of your diabetes—there are plenty of adaptive methods available to help you do it on your own.
For instance, reminders might serve as helpful reminders to take insulin. Continuous glucose monitoring may also notify loved ones if you experience dangerous swings in blood sugar.
In addition, there are devices called insulin pumps that monitor your blood sugar and inject insulin as needed. Any of these things may aid in keeping up with your treatment and reducing the likelihood of illness.
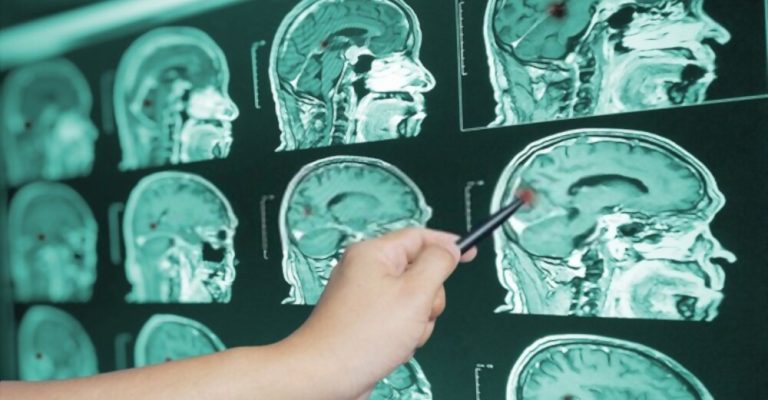
When diabetes and a brain injury both occur, the resulting complications and care requirements are one-of-a-kind. The cognitive consequences of brain damage might make monitoring sugar levels and insulin administration more challenging.
Diabetic tiredness and other complications may exacerbate the effects of brain damage. In addition, too much glucose in the blood may exacerbate existing brain damage. Luckily, recent developments in diabetes therapy have made it much simpler to mitigate the negative effects of diabetes on those who have had brain damage.
By keeping track of your blood sugar levels on a regular basis, you may prevent potentially fatal complications, including diabetic coma and seizures. If you’re having trouble keeping track of your diabetes and brain damage, it may be time to see an endocrinologist for guidance.
The co-occurrence of diabetes and TBI concerns for a number of reasons beyond just short-term physical effects; it also creates long-term psychological struggles. For example, people with both conditions often experience cognitive difficulties that interfere with everyday tasks such as memory retention and recall, making education and employment challenging.
Furthermore, mental health issues like depression and anxiety may become more prominent due to difficulty adjusting to traumatic events such as car accidents or falls that lead to a head injury.
It is crucial for medical professionals handling patients with this dual diagnosis to understand the relationship between these two illnesses to provide effective treatment plans tailored specifically for each individual. While there is no specific method for preventing or treating this dual health issue at present, further research into causes and treatments could help reduce incidences of both diseases in tandem.