According to the National Spinal Cord Injury Association, as many as 450,000 people in the United States are living with a spinal cord injury (SCI)
Spinal cord injuries are commonly seen in traumatic incidents such as gunshot, motor vehicle accidents, falls, etc. These injuries can result in various symptoms ranging from sensory symptoms such as pain, numbness, tingling, etc., to motor control deficits such as paralysis. To understand spinal cord injury and its management, you should first know the structure and function of the spinal cord.
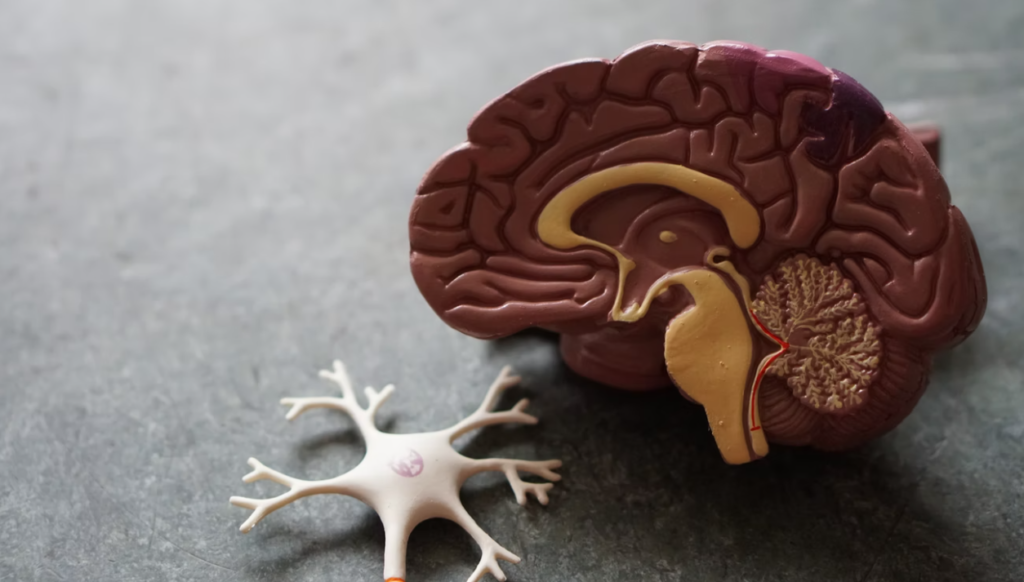
The spinal cord is a structure made up of neurons (cells) that connects your brain to the rest of your body. It lies within the center of your body and is present inside your spine (vertebral column). It is the continuation of your brain and starts from the point where the brain ends (beneath the skull). It then runs down in your spine and transmits signals from the brain to the rest of your body.
So if you want to move your hand to pick up a glass, your brain will generate a motor signal. This signal will travel down the spinal cord and ultimately reach your muscles via nerves originating from your spinal cord. Not only this, but the spinal cord also serves the function of carrying sensory signals to your brain. You can feel pain only when this sensation is conveyed to the brain via sensory nerves to the spinal cord to your brain.
This helps to understand that signal transmission is affected if the spinal cord is damaged, resulting in several sensory and motor symptoms.
Here we will focus mainly on traumatic spinal cord injury.
Trauma to the spinal cord can result in a variety of injuries. Spinal cord injuries are divided into several types based on the etiology and location of spinal cord injury.
Spinal cord injury (SCI), in which there is an injury to only one-half of the spinal cord, is called Brown Sequard Syndrome.
This injury commonly occurs because of penetration wounds such as gunshot or stab wounds.
In this type of spinal cord injury, the anterior part of the spinal cord is damaged. This commonly occurs because of hyper-flexion of the spine at the neck that disrupts the blood supply of the anterior region coming from the anterior spinal artery.
This is the most common syndrome associated with spinal cord injuries. In this type of spinal cord injury, the central part of the spinal cord is damaged due to hyper-extension of the spine at the neck. It is also associated with congenital narrowing of the spinal canal.
This injury affects the terminal part of the spinal cord, i.e., Cauda Equina. It results from herniation of lumbar discs (outward movement of discs present between lumbar vertebrae). It can also occur due to traumatic injury in the lower back.
The signs and symptoms of spinal cord injury depend upon the type of injury. Some common symptoms of spinal cord injuries are as follows.
The management of spinal cord injury is divided into the following sections.
Let’s have a look at each section one by one.

It is necessary to immobilize the spine if you suspect spinal cord injury due to trauma to your vertebrae/spine. This is important because the injury can get worse if the patient is handled carelessly. Immobilization is achieved by using several braces such as soft and hard collars, Sterno-Occipital Mandibular Immobilization (SOMI) device, Halo vest, etc.
Surgery is indicated following spinal cord injury to remove any foreign objects or ruptured discs, reduce fractured vertebrae, and decompress the spinal cord. Not all spinal cord injuries require surgical management, and some injuries can be managed non-operatively.
Steroids play an essential role in suppressing secondary events following spinal cord injury and are widely used in SCI management. Several other drugs such as NSAIDs, Gabapentin, antidepressants are also used in SCI management.

Physiotherapy management plays a crucial role during sub-acute and chronic phases of spinal cord injuries. It involves respiratory muscles training (injury at cervical level), muscles strengthening and stretching exercises, balance and coordination exercises, gait training, etc.
It consists of the maximum protection phase, intermediate protection phase, and minimum protection phase. Outcomes of physiotherapy management depend upon the level of spinal cord injury—the higher the level of injury, the poorer the outcomes. Nearly 25% of spinal cord injury patients cannot ambulate independently if the cervical spine is involved.
Like the treatments mentioned above, orthotics management plays a vital role in managing spinal cord injury in acute, sub-acute, and chronic phases of recovery.
Orthoses help stabilize the spine so that the healing is not affected by unnecessary spine movements. They also provide support to the body that helps in functional rehabilitation.
Individuals with spinal cord injury at the cervical (neck) level are instructed to wear a halo brace that immobilizes the neck region. For managing the injuries involving the neck and upper back, cervical-thoracic orthosis (CTO) is recommended. Similarly, Thoraco-Lumbar-Sacral Orthosis (TLSO) covers your whole back.
Lower limb orthoses such as Knee-Ankle-Foot Orthosis (KAFO) or Hip-Knee-Ankle-Foot Orthosis (HKAFO) are also used for assisting in ambulation following spinal cord injuries.
No matter which level is involved, spinal cord injury management is always multi-disciplinary and involves several healthcare professionals. Early detection of an injury is always a key to achieving better outcomes.